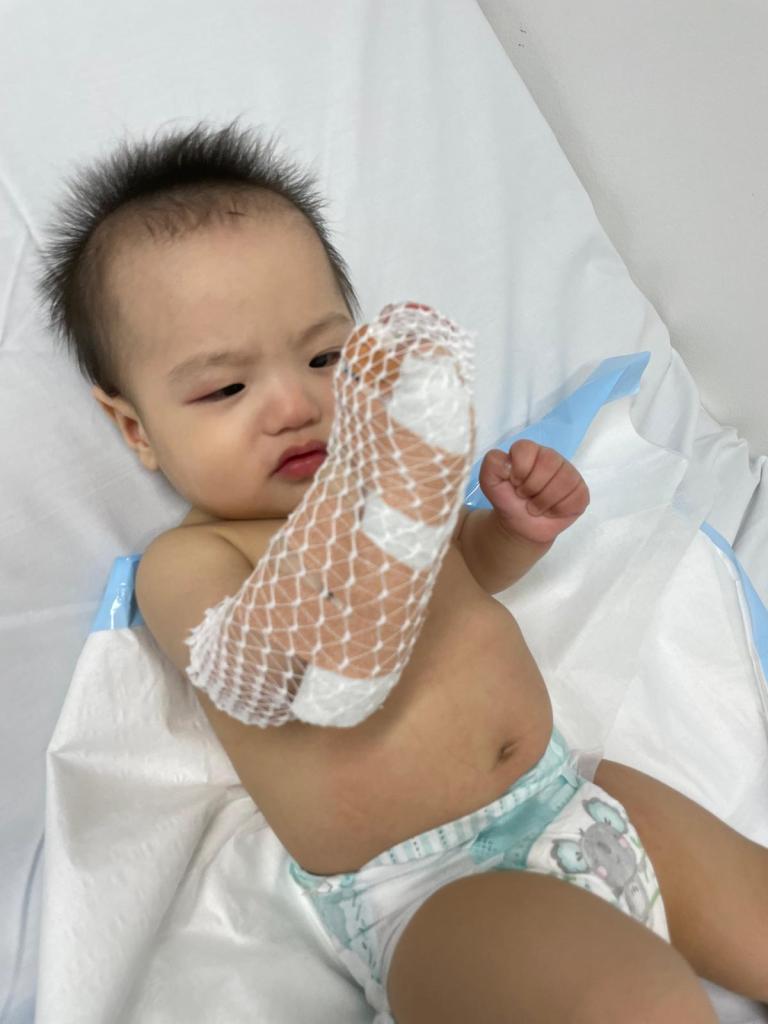
My son, Matthew was diagnosed with Kawasaki Disease in January 2022 when he was barely 7 months old.
In the afternoon of 8 January 2022, he developed a high fever which refused to budge with alternating doses of paracetamol and ibuprofen. At the time, our GP was reluctant to see him in person despite returning negative COVID tests because his symptoms overlapped with COVID symptoms and we were right in the middle of the first Omicron wave.
The GP advised us that the magic number for fever before the hospital would take us was 5 days and if he was not better by then to take him to the ED.
Over the next few days, he became increasingly unwell and more irritable. On 11 January 2022, the 4th day of fever, he developed a rash which started on his torso. The following day, his hands and feet turned a bit red.
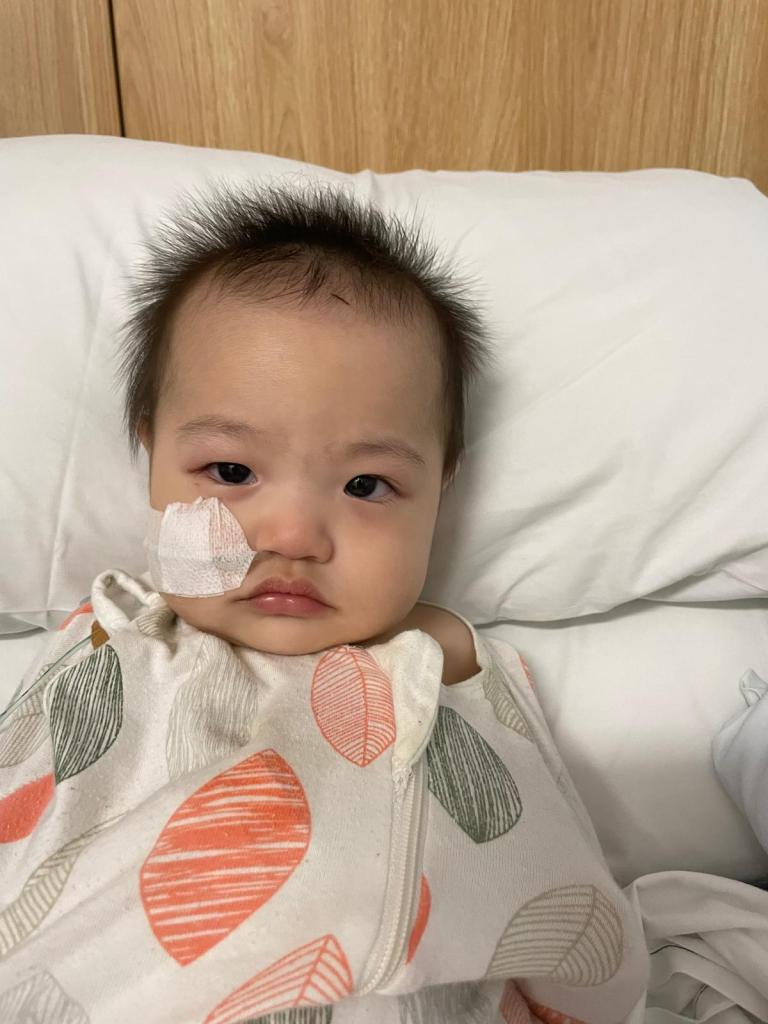
We had a few Telehealth appointments where I would be holding him up to my laptop camera hoping that the rashes that had developed on his torso would be visible to the doctor. One of the GPs we saw suggested it may be Roseola but the rash and fever were concurrent. In Roseola, typically, the rash appears after the fever breaks. Before we could even take him to the ED, we had to get him to a drive through PCR COVID testing site and wait for the results so that we could be admitted to the non-COVID ward.
Finally, on 13 January 2022, we took him to the ED at RPA as he was no longer eating or drinking and barely had any wet nappies. By this stage, although the rashes on his torso had faded, his face had red blotches, his eyes were pinkish and his lips were much redder than usual.
At the ED, they tried to get blood and urine samples and ordered chest X-rays. A spinal tap was also mentioned. It was the first doctor that we saw, an intern actually, who warned me that it may be Kawasaki Disease. I’d not heard of Kawasaki Disease before so I was quickly googling this while waiting for other doctors to see us. However, the registrar who finally admitted us was convinced he had pneumonia and put him on a cocktail of antibiotics straight away.
The next few days were a whirlwind of constant anxiety, and more blood draws, swabs and temperatures that just refused to come down. His inflammatory markers were through the roof – along with increasing platelets. The blood cultures and swabs were all returning negative. He’d also started having diarrhoea although this was dismissed as a side effect of the antibiotic cocktail.
By this stage, I’d read more about Kawasaki Disease and was in constant contact with my aunt who works overseas as a paediatrician. I was well aware that the 10 day treatment window was fast approaching. The team overseeing my son at RPA still had no answers for me so I had to keep reminding them of the possibility of a Kawasaki Disease diagnosis.
Finally, late on the 9th day of fever, the consultant signed off on the IVIg treatment on the basis that they had spoken with infectious disease specialists who agreed that it was not an infection and that although they were not convinced that it was Kawasaki Disease, it could not be excluded. After a harrowing 1 hour where they couldn’t get the IV line in, they finally started the infusion overnight. I did not sleep a wink overnight as I was so worried that the IV would slip out and they would have to start over. Within an hour or two of starting the infusion, his temperatures came down miraculously and stayed down and the next morning he was back to his happy and smiling self.
We were sent for our first echocardiogram at Sydney Children’s on 18 January 2022 and thankfully, no aneurysms were seen. We were discharged on the same day and prescribed aspirin daily. Interestingly, his fingers and toes started to peel on this day.
At the 3 month follow up, his left main coronary artery was found to be dilated and this remained the case until 18 months later.
I think even at discharge, the medical team didn’t believe that he had Kawasaki Disease and they reluctantly diagnosed him with atypical Kawasaki Disease because they couldn’t find any other explanation but I’m glad they finally gave him the IVIg treatment when they did.
It was an extremely traumatic experience and I wish they’d taken the first doctor’s diagnosis seriously. I’m so grateful that she mentioned it to me in the first place so that I could look out for more symptoms and that I had my aunt as a support system so that I could advocate for Matthew and keep bringing it up with the medical team.